Polyarteritis nodosa (PAN) is a rare disease caused by inflammation of the blood vessel (“vasculitis”) that causes organ system injury. Nerves, intestinal tract, heart, and joints are the areas most commonly affected by PAN. PAN may also affect the kidney’s blood vessels, resulting in high blood pressure and kidney function damage. It is a systemic necrotizing inflammation of the blood vessels (vasculitis) that affects medium-sized muscle arteries, typically involving the arteries of the kidneys and other internal organs, which generally inhibits the drainage of the lungs. PAN affects only medium-sized blood arteries, which was first described by Kussmaul and Maier in 1866. A patient’s autopsy with fever, weight loss, abdominal pain, and polyneuropathy showed regions of focal inflammatory exudations that produced visible nodules across medium-sized artery vessels.
Table of Content
- Polyarteritis Nodosa Symptoms
- Causes of Polyarteritis Nodosa
- Diagnosis of Polyarteritis Nodosa
- Treatment of Polyarteritis Nodosa
What Is Vasculitis?
Vasculitis is a general term relating to blood vessel inflammation. The blood vessel may become compromised when inflamed and expand in length, which may lead to aneurysms, or become so thin that it splits into the tissue that it bleeds. Vasculitis can also cause the blood vessel to close so that the lungs are weakened by the lack of oxygen and blood-supplied nutrients. PAN affects only medium-sized blood vessels.
Polyarteritis Nodosa Symptoms
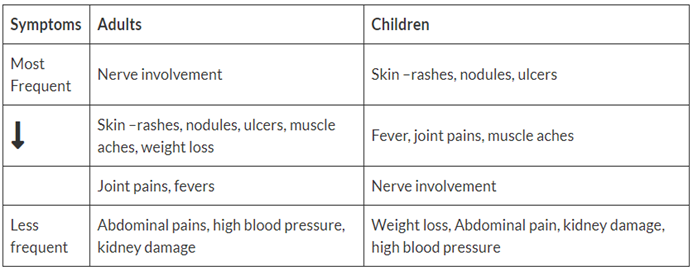
Because there may be several different organ systems involved, PAN can have a wide range of symptoms. Patients with PAN may feel sick and tired in general, have a fever, or lose appetite and weight. Some may have symptoms related to areas of involvement such as muscle and/or joint pain, skin sores that may be present as rough nodules or ulcers, abdominal pain or blood in stools which occur as a result of involvement in the intestinal tract, or shortness of breath or chest pain from heart disease. High blood pressure is common in PAN and is usually caused by reduced blood flow to the kidneys due to vasculitis.
PAN’s symptoms include:
- a weakened appetite
- abrupt loss of weight
- abdominal pain
- muscle and joint aches
- excessive fatigue
- fever
PAN influences the nervous systems of nearly 70% of people, according to Johns Hopkins. PAN can induce seizures and cause neurological problems after two to three years if left untreated. It results in reduced alertness and cognitive dysfunction. PAN often affects the skin on the legs. Skin lesions are very common.
Causes of Polyarteritis Nodosa
There is no knowledge of the exact cause of polyarteritis nodosa. No predisposing factor was observed in most cases. Unidentified diseases of bacteria and/or viruses can be a cause. In drug abusers, particularly those who use amphetamines, and in patients with hepatitis B (liver infection), polyarteritis nodosa was observed. (For more information on this disease, pick “Hepatitis B” as the Rare Disease Database search term.) This condition was also associated with an allergic reaction to certain medications and vaccines. PAN’s cause is unknown. PAN is not a cancer form, it is not contagious, and it usually does not occur in families. Research laboratory evidence strongly supports the immune system playing a critical role in PAN, causing inflammation and damage to the blood vessel and tissue. PAN is strongly associated with infection with hepatitis B. Since the vaccine for hepatitis B was established, PAN rates have significantly decreased.
Diagnosis of Polyarteritis Nodosa
PAN is a complex condition requiring multiple studies before a confirmatory diagnosis can be done by the physician. The doctor will probably prescribe a complete blood count to test the red blood cells and white blood cells count as a primary investigation.
A doctor may diagnose PAN based on medical history and symptoms of PAN.
- Physical examination may be required to detect affected organs and to rule out other similar diseases.
- Blood tests and a urinalysis may be done to understand affected organs and the occurrence of inflammation.
- X-rays, CT scans, or MRI scans can indicate anomalies in affected areas.
After the diagnosis of suspected PAN, confirmation can be done by arteriogram or a biopsy. In the arteriogram procedure, a dye is injected into the bloodstream, it enables visualisation of blood vessels and an indication of vasculitis or narrowing of blood vessels. A biopsy of an affected area can confirm the presence of vasculitis in the tissue. Biopsies and arteriograms are only done, where there are abnormal findings in a pathological test or imaging studies.
Treatment of Polyarteritis Nodosa
Treatment of PAN involves a combination of drugs like corticosteroids, immune suppressants and antiviral drugs.
Corticosteroids reduce inflammation caused due to PAN but may have various side effects if administered orally. Corticosteroids help in preventing arteries from the attack of the immune system is severe conditions. Corticosteroids are taken with immunosuppressive drugs. Antiviral medication is administered in hepatitis infection. Patients with PAN with essential activity in the organ system are generally treated with a corticosteroid such as prednisone or prednisolone in conjunction with other immunosuppressive drugs such as cyclophosphamide (Cytoxan ®). Cyclophosphamide is given for certain types of cancer at high doses as a cure and is therefore often referred to as “chemotherapy.”
Discover other interesting concepts important for NEET only at BYJU’S.
Read more:

Comments